Olivia was a web designer. However, long hours in front of her laptop took their toll: Olivia developed pain in her hands and wrists. She was advised to take a two-week break from work and do some hand stretches.
After two weeks, she did not return to work. “I’m afraid that typing will cause my pain to flare up again and this time it won’t go away. Then I’ll end up completely disabled and starve to death because I won’t be able to hold a glass of water. After all, I tried playing a video game yesterday and my wrists were kind of uncomfortable. I think they’re permanently damaged.”
If you’ve ever had a patient like Olivia, you know how hard it can be to help them. In this article, we’ll explain this type of patient behavior using the fear-avoidance model and discuss some of the best treatment options.
What is the fear-avoidance model?
The fear-avoidance model used in physical therapy describes how people can develop chronic pain as a result of avoidant behavior caused by fear.
Fear and avoidance are normal, healthy responses to acute pain. After all, it’s a good idea to be defensive and avoid movement right after an injury.
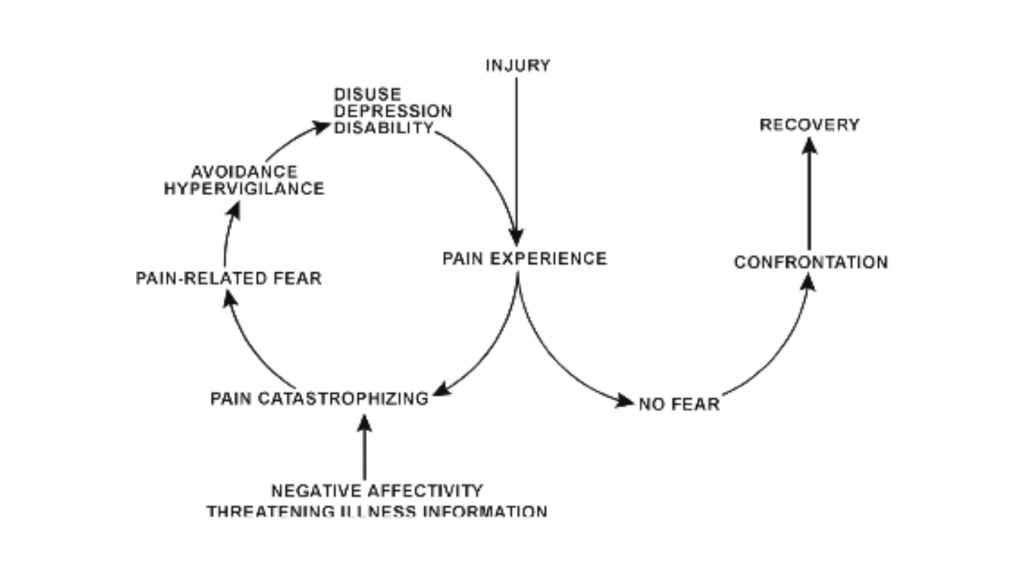
As the injury begins to heal and the pain becomes chronic, there are two possible outcomes. Ideally, the injured person will accept the pain and focus on regaining their independence. In most cases, they will recover quickly.
The other outcome is less optimistic. If the injured person has a highly negative attitude towards pain (known as pain catastrophizing, a type of catastrophic thinking), they will develop an intense fear of pain and start avoiding any activities that might cause it (“squats make my knees hurt”, “typing gives me wrist pain” etc). This leads to a host of negative consequences. The affected part of the body becomes even weaker because it’s no longer used, leading to even more pain and even more fear. In short, it’s a vicious circle of physical and emotional pain that fuel each other.
What exactly is catastrophic thinking?
We’ve already mentioned catastrophic thinking when describing the fear-avoidance model. But what does it mean, exactly?
Generally, catastrophic thinking (or pain catastrophizing) can be defined as an exaggerated negative orientation toward pain-related stimuli. There are three commonly accepted dimensions of this negativity:
- rumination (constant negative thoughts about pain).
- magnification (seeing every pain as a threat).
- helplessness (a perceived lack of control over pain).
Catastrophic thinking is linked to increased pain intensity, decreased physical function and a higher likelihood of long-term disability. So once you notice that a patient is prone to pain catastrophizing, consider referring them to a psychotherapist who specializes in chronic pain or try to help them on your own. For example, simply explaining the fear-avoidance model to a patient can help them change the way they think about their pain.
Is there a way to measure fear-avoidance beliefs?
There are several questionnaires that healthcare professionals (including you) can use to evaluate the intensity of your patients’ fear avoidance beliefs.
The Fear-Avoidance Belief Questionnaire (FABQ) was developed for low back pain, but it can be used for any kind of musculoskeletal pain. It takes about 10 minutes to complete and consists of 16 questions that gauge a patient’s attitude towards their work and physical activity in general.
The Tampa Scale of Kinesiophobia (TSK) is a questionnaire that consists of 17 items and measures the fear of movement. It can be used with patients who suffer from back pain, neck pain, and other kinds of chronic musculoskeletal pain.
The Pain Anxiety Symptom Scale (PASS) is another well-established tool for measuring fear and anxiety responses to pain.
Last but not least, the Fear-Avoidance Components Scale (FACS) is a recently developed scale that measures various aspects of fear avoidance beliefs, including pain catastrophizing.
All of these questionnaires are short and rarely take more than 15 minutes to complete so they won’t take up an entire appointment. However, they can give you valuable insights into your patients’ attitudes towards pain.
Are there any proven treatment options?
An interdisciplinary approach can be very effective when treating chronic pain. If you feel that your patient needs help with the mental aspects of their pain, it’s a good idea to refer them to a mental health professional.
Here are several approaches that can be helpful in overcoming chronic pain and reducing fear-avoidance behaviors:
- Graded exposure involves encouraging patients to try fear-inducing activities gradually so that their anxiety doesn’t get out of control and they come to realize that movement isn’t as catastrophically painful as they imagined it to be.
- Cognitive-behavioral therapy (CBT) helps people understand the negative thought patterns that shape their daily life and replace them with more helpful thought patterns.
- Acceptance and commitment therapy (ACT) can help your patients come to terms with their condition and lead a happy, fulfilled life despite chronic pain.
- Mind-body approaches including guided visualizations and meditation can reduce the anxiety caused by chronic pain.
- Yoga can have a profound effect on mental and physical well-being alike. The stretching and strengthening exercises help alleviate chronic pain whereas the focus on mindfulness helps reduce anxiety and clear the mind from intrusive thoughts.
Distraction is another powerful tool for reducing chronic pain and forgetting about pain-related fears. One way to keep the patient distracted while performing potentially painful movements is occupy their mind with a video game or a VR experience.

Bonus: How do I help my patients cope with the fear of falling?
Another prominent example of the fear-avoidance model is the fear of falling. It is one of the most debilitating fears related to movement. After all, it can prevent people from continuing their normal activities or even leaving their home.
The fear of falling can become a self-fulfilling prophecy. When a person avoids walking or standing because of their fear, their sedentary lifestyle makes them weaker and less coordinated – and, therefore, even more susceptible to falls and long-term disability.
However, as a physical therapy professional, you can help your patients break this vicious circle of fear and avoidance by adapting the rehabilitation program to their physical and emotional needs. Here are some things you can focus on:
- Weight-shifting exercises that help improve confidence when walking.
- Strength and mobility training.
- Practicing the movement patterns of everyday activities (picking objects off the floor, climbing the stairs, etc) to improve motor coordination and gradually expose the patient to activities they find fear-inducing.
- Strengthening exercises that don’t involve walking or balancing (water aerobics, using an exercise bike, etc).
- Relaxation and distraction techniques to help control anxiety.
Conclusion
The fear-avoidance model offers a solid explanation of why some people recover quickly while others seem to get stuck in an endless cycle of fear and chronic pain. Observe your patients carefully and help them overcome pain catastrophizing and avoidance with evidence-based treatments like CBT or ACT. In addition, you can help them keep their mind occupied by offering video games and other fun distractions to cope with their pain.